See attachment
You are using an out of date browser. It may not display this or other websites correctly.
You should upgrade or use an alternative browser.
You should upgrade or use an alternative browser.
COMLEX Help with EKG question
- Thread starter person011
- Start date
- Joined
- Aug 20, 2012
- Messages
- 814
- Reaction score
- 231
Let's break this down.
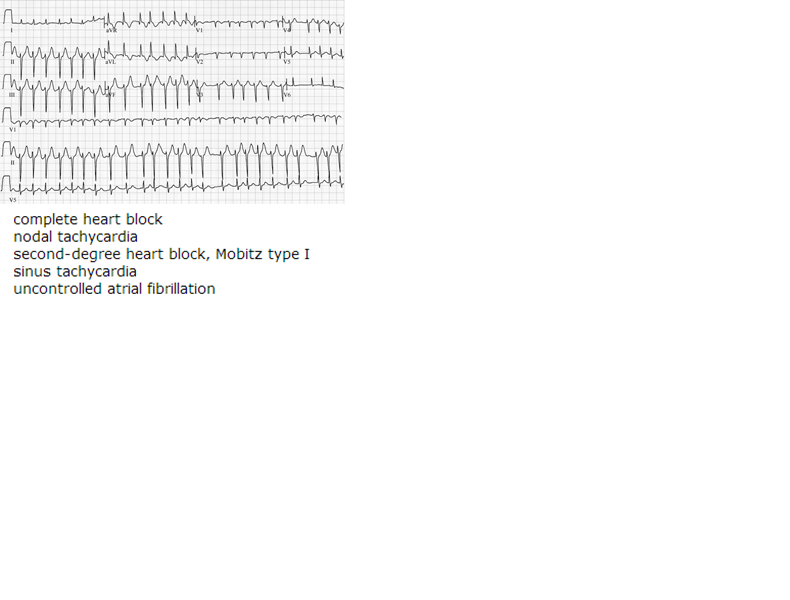
1. It appears to be a more or lessregular irregular rhythm.
2. The rate is around 150bpm (300/2 large squares)
3. The axis is possibly deviated towards the right. (I and aVF in opposite directions, lead II negative)
4. The QRS complex is narrow
5. The P wave seems to be hidden or absent (although the picture is really too small to appreciate this, I will explain this later)
6. No significant ST changes
7. T wave inversions
8. No other artifacts
Now let's look at your options:
a. Complete heart block: Not likely because of 2. Complete heart block is characteristically a bradycardia due to the idio-ventricular rhythm, with the P waves and QRS complexes having their own separate (but regular) rhythms.
b. Nodal tachycardia:Most Not likely, because of 1. AVNRT is a narrow complex tachycardia, with a high ventricular rate characteristic (>120) of an SVT, but it's strikingly regular in its rhythm, unlike this ECG.
c. Second degree heart block, Mobitz type I: Not likely because of 2. Also, the PR interval would progressively prolong until a dropped beat occurred, characteristic of Mobitz type I.
d. Sinus tachycardia: Possible, although 2 goes against it. Sinus tachycardia tends to have a rate not higher than 120bpm.
e. Uncontrolled atrial fibrillation:Not Most likely because of 1, 2 and 5. Atrial fibrillation is characteristically an irregular rhythm with an uneven baseline and absent P waves. Uncontrolled atrial fibrillation indicates a rapid ventricular rhythm RVR (>140 bpm) which is seen on this ECG.
The initial segments of the limb leads illustrate the irregularity of the rhythm (which I discounted at first). For the USMLE irregular rhythm with absent P waves is quite characteristic of atrial fibrillation.
Now for some explanation. In an AVNRT there exist two pathways in the right atrium close to the AV node, the fast and the slow pathway that allow both anterograde and retrograde conduction of electrical impulses (each one conducting in opposite directions). Because of this, it is possible to set up a re-entry rhythm (hence the R in AVNRT) that can cause an SVT (any pacemaker above the bundle of His is called an SVT) because the AV node which usually creates the delay is not part of this pathway. The most famous SVT is that of Wolff Parkinson White syndrome where the characteristic finding (apart from the ones already mentioned) is the slurring of the QRS upstroke - the delta wave. It must be remembered that the pathway here is different from AVNRTs.
1. It appears to be a more or less
2. The rate is around 150bpm (300/2 large squares)
3. The axis is possibly deviated towards the right. (I and aVF in opposite directions, lead II negative)
4. The QRS complex is narrow
5. The P wave seems to be hidden or absent (although the picture is really too small to appreciate this, I will explain this later)
6. No significant ST changes
7. T wave inversions
8. No other artifacts
Now let's look at your options:
a. Complete heart block: Not likely because of 2. Complete heart block is characteristically a bradycardia due to the idio-ventricular rhythm, with the P waves and QRS complexes having their own separate (but regular) rhythms.
b. Nodal tachycardia:
c. Second degree heart block, Mobitz type I: Not likely because of 2. Also, the PR interval would progressively prolong until a dropped beat occurred, characteristic of Mobitz type I.
d. Sinus tachycardia: Possible, although 2 goes against it. Sinus tachycardia tends to have a rate not higher than 120bpm.
e. Uncontrolled atrial fibrillation:
The initial segments of the limb leads illustrate the irregularity of the rhythm (which I discounted at first). For the USMLE irregular rhythm with absent P waves is quite characteristic of atrial fibrillation.
Now for some explanation. In an AVNRT there exist two pathways in the right atrium close to the AV node, the fast and the slow pathway that allow both anterograde and retrograde conduction of electrical impulses (each one conducting in opposite directions). Because of this, it is possible to set up a re-entry rhythm (hence the R in AVNRT) that can cause an SVT (any pacemaker above the bundle of His is called an SVT) because the AV node which usually creates the delay is not part of this pathway. The most famous SVT is that of Wolff Parkinson White syndrome where the characteristic finding (apart from the ones already mentioned) is the slurring of the QRS upstroke - the delta wave. It must be remembered that the pathway here is different from AVNRTs.
Last edited:
I don't think so actually. I don't see why that would not be afib rvr. If you are saying its SVT w/ some dropped beats, the R-R would be mostly equal with minimal variability. That's not what I see on there.
Also no P waves at all
Also no P waves at all
- Joined
- Aug 20, 2012
- Messages
- 814
- Reaction score
- 231
Looking at the rhythm again, you're right. It is irregular, and Afib with RVR definitely fits the pattern. The no P waves bit can be argued in the favour of an SVT as well though, it's dependent on the timing of atrial depolarisation. I'll modify my original response accordingly.I don't think so actually. I don't see why that would not be afib rvr. If you are saying its SVT w/ some dropped beats, the R-R would be mostly equal with minimal variability. That's not what I see on there.
Also no P waves at all
Glad you agree... Mostly bc i was starting to question my understanding of SVT!
On p waves though, there should be some degree of synchronized atrial activity (biphasic, flipped, superimposed)
Av nodal you would think it would be retrograde conduction and therefore flipped, as i understand it
On p waves though, there should be some degree of synchronized atrial activity (biphasic, flipped, superimposed)
Av nodal you would think it would be retrograde conduction and therefore flipped, as i understand it
- Joined
- Aug 20, 2012
- Messages
- 814
- Reaction score
- 231
It can be hidden in the QRS when superimposed. You can often see it right after the QRS on the ST segment, or a little further away depending on which pathway conducts retrograde. It can even be on the R wave creating a false R'. And yes, being retrograde, it will be inverted if present.
Similar threads
- Replies
- 2
- Views
- 1K
